Patient Portals and MACRA / MIPS / Meaningful Use
Patient Portals and MACRA / MIPS / Meaningful Use
Meaningful Use
The Centers for Medicare & Medicaid Services (CMS) established the EHR Incentive Programs (also known as meaningful use) in 2011. The EHR Incentive Program encourages Eligible Professionals (EPs), Critical Access Hospitals (CAHs), and eligible hospitals to execute, manage, and prove meaningful use of Certified Electronic Health Record Technology (CEHRT).
Participants are scored on four objectives¹ (Electronic Prescribing, Health Information Exchange, Provider to Patient Exchange, and Public Health and Clinical Data Exchange). Depending on their score, participants can receive incentive payments/penalties.
There have been three stages to meaningful use:
- Stage 1 (start date 2011): Data capture and sharing
- Stage 2 (start date 2014): Advanced clinical processes
- Stage 3 (start date 2017): Improved outcomes
In 2018, Meaningful Use (MU) became known as Promoting Interoperability Programs². Participants can attest to the Medicare Promoting Interoperability Programs or Medicaid Promoting Interoperability Programs.
MACRA
On April 16, 2015 The Medicare Access and CHIP Reauthorization Act of 2015 (MACRA) was signed into law. Under MACRA, providers caring for Medicare beneficiaries will be paid based on the quality of the care they provide.
MIPS
Merit Based Incentive Payments System (MIPS) is a payment track created under MACRA. It aims to link payments to the quality of care provided, improve care processes and health outcomes, increase the use of healthcare information, and reduce the cost of care.
What is the difference between Meaningful Use Stage 3 (MU3), MACRA, and MIPS?
| Meaningful Use - Stage 3 (MU3) | MACRA | MIPS | |
|---|---|---|---|
| Function | Healthcare organizations wanting to receive incentive payments through CMS must demonstrate meaningful use of an electronic health record to improve health outcomes. Also, this rule modified MU2 to ease reporting requirements and align with other CMS programs. | Provides new ways to pay physicians for caring for Medicare beneficiaries. Under MACRA, participating providers will be paid based on the quality and effectiveness of the care they provide. | Provides new ways to pay physicians for caring for Medicare beneficiaries. Under MACRA, participating providers will be paid based on the quality and effectiveness of the care they provide.
|
| Initiation Date | 2015 | 2015 | 2017 |
| Governing Authority | CMS & OMS | CMS | CMS |
What was the timeline of Meaningful Use and MACRA/MIPS programs?
2009
- The American Reinvestment and Recovery Act (ARRA) was enacted.
- The accompanying Health Information Technology for Economic and Clinical Health (HITECH) Act was also enacted.
2011
- EHR Incentive Programs (Also known as Meaningful Use) Start January 2011
- Meaningful Use Stage 1 enacted
- January 2011 Start of EHR Incentive Programs registration
- April 2011 Start of the Medicare EHR Incentive Program attestation
- May 2011 Start of EHR Incentive Payments
- November 30, 2011, Last day for eligible hospitals and CAHs to register and attest to receive an Incentive Payment for 2011
2012
- FEBRUARY 29, 2012 Last day for EPs to register and attest to receive an Incentive Payment for 2011.
2014
- Meaningful Use Stage 2 enacted.
- Last year to initiate participation in the Medicare EHR Incentive Program.
2015
- The Medicare Access and CHIP Reauthorization Act of 2015 (MACRA) was signed into law on April 16, 2015.
- Modified Stage 2
- In October 2015, CMS released the Modifications to Meaningful Use in 2015 through 2017 final rule³, which modified Stage 2 requirements to streamline reporting requirements on measures.
- Medicare payment adjustments begin for EPs and eligible hospitals that are not meaningful users of EHR technology.
2016
- Last year to receive a Medicare EHR Incentive Payment.
- Last year to initiate participation⁴ in the Medicaid EHR Incentive Program.
2017
- The first performance period for MACRA.
- Meaningful Use Stage 3 enacted.
- QPP (Quality Payment Program)⁵ started on January 1, 2017.
2018
- EHR Incentive Programs changed its name to Promoting Interoperability Programs⁶.
- Eligible Practitioners and Eligible Clinicians who previously participated in Medicare Promoting Interoperability Programs are now required to report for QPP.
2020
- All EPs must attest to Stage 3 MU objectives Eligible Professionals (EPs): December 1, 2020, to February 28, 2021.
2021
- Promoting Interoperability: Medicaid⁷ will end on September 30, 2021. No payments⁸ will be made to any provider after 2021. There is a 90-day reporting period for both EHR and eCQM for all EPs⁹ to meet the incentive payment deadline of December 31, 2021.
- Promoting Interoperability: Medicare¹⁰ incentive program will end on September 30, 2021, and any outstanding incentive payments will stop. Penalty payment adjustment for non-attestation will stay in place.
- March 1, 2021 Deadline to submit 2020 data for the Medicare Promoting Interoperability Program.
2022
- Participants of the Medicare Promoting Interoperability Program¹¹ (eligible hospitals and CAHs) are required to report for any continuous 90-day period attesting to CMS.
What is the financial impact of compliance with MU?
Under the Medicaid Electronic Health Record Incentive Payments for Eligible Professionals¹², to receive the maximum incentive payments, participants must meet the 30 percent patient volume requirement. Participants who achieved between 20-30 percent patient volume will receive two-thirds of the total incentive payment.
| Year | Medicaid EPs Who Adopted In | |||||
|---|---|---|---|---|---|---|
| 2011 | 2012 | 2013 | 2014 | 2015 | 2016 | |
| 2011 | $21,250 | |||||
| 2012 | $8,500 | $21,250 | ||||
| 2013 | $8,500 | $8,500 | $21,250 | |||
| 2014 | $8,500 | $8,500 | $8,500 | $21,250 | ||
| 2015 | $8,500 | $8,500 | $8,500 | $8,500 | $21,250 | |
| 2016 | $8,500 | $8,500 | $8,500 | $8,500 | $8,500 | $21,250 |
| 2017 | $8,500 | $8,500 | $8,500 | $8,500 | $8,500 | |
| 2018 | $8,500 | $8,500 | $8,500 | $8,500 | ||
| 2019 | $8,500 | $8,500 | $8,500 | |||
| 2020 | $8,500 | $8,500 | ||||
| 2021 | $8,500 | |||||
| Total | $63,750 | $63,750 | $63,750 | $63,750 | $63,750 | $63,750 |
Note: the total for pediatricians who meet the 20 percent patient volume but fall short of the 30 percent patient volume is $14,167 in the first year and $5,667 in subsequent years. This adds up to a maximum Medical EHR incentive payment of $42,500 over a six-year period.
Under Medicare¹⁴, the EHR incentive payment amount is equal to 75 percent* of an Eligible Professional's Medicare physician fee schedule allowed charges submitted not later than two months after the end of the calendar year. *subject to an annual limit.
What are the timeline/deadlines of MU?
Medicaid
Reporting period: a 90-day period within the calendar year. The attestation period and deadline are dependent on state Medicaid.
Medicare
Reporting period: Minimum of any continuous 90-day period, for both 2020 and 2021/ 90-day period in the calendar year 2020. March 1, 2021, is the deadline to submit 2020 data for the Medicare Promoting Interoperability Program.
How does a patient portal impact MU attestation?
All participants in the Medicaid and Medicare Promoting Interoperability Programs are required to use 2015 Edition CEHRT. Bridge is a 2015 certified patient portal; therefore, healthcare organizations can use Bridge to attest to Medicare and Medicaid Promoting Interoperability Programs.
Medicare: Eligible hospitals, CAHs, and dual-eligible hospitals attesting to Medicare Promoting Interoperability Program to CMS will be required to report on four objectives.
- Electronic Prescribing
- Health Information Exchange
- Provider to Patient Exchange
- Public Health and Clinical Data Exchange
Medicaid: Eligible professionals (EPs) and eligible hospitals are required to report on any six eCQMs¹⁷ (Electronic Clinical Quality Measures) for Medicaid Promoting Interoperability Program attestation, as well as report on at least one outcome measure.
Is MU3 still relevant/mentioned?
The term Meaningful Use is no longer used or relevant. EHR Incentive Programs (Also known as Meaningful Use) changed its name to Promoting Interoperability Programs in 2018, though some continue to refer to this as Meaningful Use Stage 3. Promoting Interoperability: Medicaid¹⁸ will end on September 30, 2021. Promoting Interoperability: Medicare¹⁹ incentive program will end on September 30, 2021, and any outstanding incentive payments will stop. Penalty payment adjustment for non-attestation will stay in place.
What is the financial impact of compliance with MACRA/MIPS?
Clinicians providing valuable patient care of high quality in compliance with MACRA/MIPS are rewarded through an increase in Medicare, while clinicians not performing to MACRA/MIPS standards will receive a reduction in Medicare payments. The MIPS eligible clinician's final score range is 0 to 100 and determines their payment adjustment.
Payment adjustments are applied based on an eligible clinician's performance two years after the performance year. MIPS participants in 2020 will receive a payment adjustment in 2022 based on 2020 data. Payment adjustments are applied only to payments made for covered professional services provided by a MIPS eligible clinician. Eligible clinician's earning incentives are effectively being paid by those receiving penalties for substandard performance.
Below we present the MIPS payment adjustments, including the maximum impact range. The history of payment adjustments, as well as predicted future payment adjustments, is included below.
Performance year - The period in which eligible clinicians collect data for the four performance categories.
Submission window - The period in which eligible clinicians submit their collected data from the performance year.
Payment adjustment year - The year that eligible clinicians' payment is either negatively or positively impacted based on their data collected in the performance year.
| Performance Year | Payment Adjustment Year | Performance Treshold | Maximun -% MIPS Penalty | Maximun +% MIPS base incentive | Maximun +% MIPS exceptional performance bonus |
|---|---|---|---|---|---|
| 2017 | 2019 | 3 | -4 | +4%*X(Actual 0.29%) | +10%*Y(Actual 1.59%) |
| 2018 | 2020 | 15 | -5 | +5%*X(CMS Predict 0.30%) | +10%*Y(Actual 1.75%) |
| 2019 | 2021 | 30 | -7 | +7%*X(CMS Predict 1.11%) | +10%*Y(Actual 3.58%) |
| 2020 | 2022 | 45 | -9 | +9%*X | +10%*Y |
| 2021 | 2023 | 50 | -9 | +9%*X | +10%*Y |
| 2022 | 2024 | 65 | -9 | +9%*X | +10%*Y |
What are the timeline/deadlines of MACRA/MIPS attestation?
- Submission Window for Performance Year 2017: January 2, 2018 - April 3, 2018. Payment adjustment year: 2019
- Submission Window for Performance Year 2018: January 2, 2019 - April 2, 2019. Payment adjustment year: 2021
- Submission Window for Performance Year 2019: January 2, 2020 - April 30, 2020. Payment adjustment year: 2022
- Submission Window for Performance Year 2020: January 4, 2021 - March 31, 2021. Payment adjustment year: 2023
- The extreme and uncontrollable circumstances application²⁰ deadline for PY 2020 is February 1, 2021, at 8 p.m. ET.
- The 2021 MIPS performance year runs from January 1, 2021, to December 31, 2021.
- Submission Window for Performance Year 2021: January 3, 2022 - March 31, 2022. Payment adjustment year: 2023
- In 2022 CMS aims to implement MIPS Value Pathways (MVPs), a new MIPS participation framework.
- Period of data collection for MIPS measures 2021.
| Quality | Improvement Activities | Promoting Interoperability | Cost | |
|---|---|---|---|---|
| Collect Data | 6 Measures | 2 and 4 activities | 6 required measures | Clinicians don't need to collect or submit any data for cost measures. |
| Period of data collection | 12-month performance period (January 1 – December 31, 2021). | The continuous 90-day period in Calendar Year | Same 90(+)-day performance period in Calendar Year 2021. | 12-month performance period (January 1 – December 31, 2021). |
What are MIPS Value Pathways (MVPs)?
MIPS Value Pathways (MVPs), are a new MIPS participation framework. MVPs aim to away from siloed reporting of measures and activities towards focused sets of measures and activities that are more meaningful to a clinician’s scope of practice that is meaningful to patient care. CMS is working with stakeholders to create a MVP reporting criteria for the year 2022.
How does a patient portal impact MACRA/MIPS attestation?
A patient portal can help participants attest for Provide Patients Electronic Access to Their Health Information, a measure of the Promoting Interoperability performance category, which makes up 25% of the MIPS final score. Bridge is a 2015 certified patient portal; therefore, healthcare organizations can use Bridge to promote interoperability for the Merit-Based Incentive Payment System (MIPS). With Bridge’s use, patients are provided timely access to view, download, and transmit their health information.
How has MIPS performance categories have changed over the years?
The table below demonstrates the change in performance categories weight over the years, including the change in the performance threshold.
| Performance Year | Quality Category % | Cost % | Promoting Interoperability % | Improvement activities % | Performance threshold |
|---|---|---|---|---|---|
| 2018 | 50 | 10 | 25 | 15 | 15 |
| 2019 | 45 | 15 | 25 | 15 | 30 |
| 2020 | 45 | 15 | 25 | 15 | 45 |
| 2021 | 40 | 20 | 25 | 15 | 60 |
| 2022 | 30 | 30 | 25 | 15 | 65 |
Is a 2015 Edition CEHRT Required for Promoting Interoperability Program?
Up until 2015, all eligible providers were required to report using 2014 Edition CEHRT. Providers could continue using a 2014 Edition CEHRT until 2018. In 2019, health care providers were required to begin using a 2015 Edition CEHRT. Participants in the Promoting Interoperability Programs (formerly known as Meaningful Use) are expected to use 2015 Edition Certified Electronic Health Record Technology (CEHRT).
What is the Cures Act?
In 2016, Congress passed the 21st Century Cures Act²² to drive the electronic access, exchange, and use of health information. The Office of the National Coordinator for Health Information Technology (ONC) Cures Act Final Rule²³ implements the interoperability provisions of the Cures Act to promote patient control over their health information. The 21st Century Cures Act aims to ensure that all parties (patients, caregivers, and healthcare providers) have appropriate access to electronic health information. The Act also promotes access to electronic health information in a secure and straightforward manner. Patients should be able to access their electronic medical records free of charge. Providers should have the freedom to choose easy to use, reasonably priced health IT tools to facilitate the best care for their patients.
How can Bridge help an organization achieve MACRA/MIPS/Cures Act compliance? Table showing how Bridge can help organizations achieve compliance.
| MACRA/MIPS | ONC's Cures Act Final Rule |
|---|---|
| Promoting Interoperability Measures | Protecting Patient Privacy and Security |
| Requirements This performance category promotes patient engagement and electronic exchange of information using Certified Electronic Health Record Technology (CEHRT). | The rule supports secure patient access to their electronic medical record data. Patients will be able to use applications they authorize to receive data from their medical records. OAuth 2 is used to authorize applications. Promoting the Ability to Shop for Care and Manage Costs ONC's Cures Act Final Rule looks to expand patient and payer choice in health care by increasing data availability to support insights about care quality and costs. Making Patient Data Requests Easy and Inexpensive Modern technology allows clinicians and hospitals to easily provide patients with access to their information in a fully automated, low-cost manner. Patients will be able to access their health information from an app of their choice. Secure, standardized Application Programming Interfaces (APIs) allow for this access without special effort on the clinician's part. |
Bridge Patient Portal was certified on 16 different EHR criteria, representing a significant range of functionality for an EHR-independent 3rd party patient portal solution. Bridge Patient Portal meets the following 2015 Edition ONC Health IT Certification Criteria:
- Meets 170.315 (d)(1): Authentication, Access Control, Authorization
- Meets 170.315 (d)(2): Auditable Events and Tamper-Resistance
- Meets 170.315 (d)(3): Audit Report(s)
- Meets 170.315 (d)(5): Automatic Access Time-out
- Meets 170.315 (d)(6): Emergency Access
- Meets 170.315 (d)(7): End-User Device Encryption
- Meets 170.315 (d)(9): Trusted Connection
- Meets 170.315 (e)(1): View, Download, and Transmit to 3rd Party
- Meets 170.315 (e)(2): Secure Messaging
- Meets 170.315 (g)(1): Automated Numerator Recording
- Meets 170.315 (g)(4): Quality Management System
- Meets 170.315 (g)(5): Accessibility-Centered Design
- Meets 170.315 (g)(6): Consolidated CDA Creation
- Meets 170.315 (g)(7): Application Access - Patient Selection
- Meets 170.315 (g)(8): Application Access - Data Category Request
- Meets 170.315 (g)(9): Application Access - All Data Request
How the Cures Act is related to MACRA/MIPS
Congress officially passed the 21st Cures Act in 2016 to continue the promotion of EHR adoption initiated by MACRA.
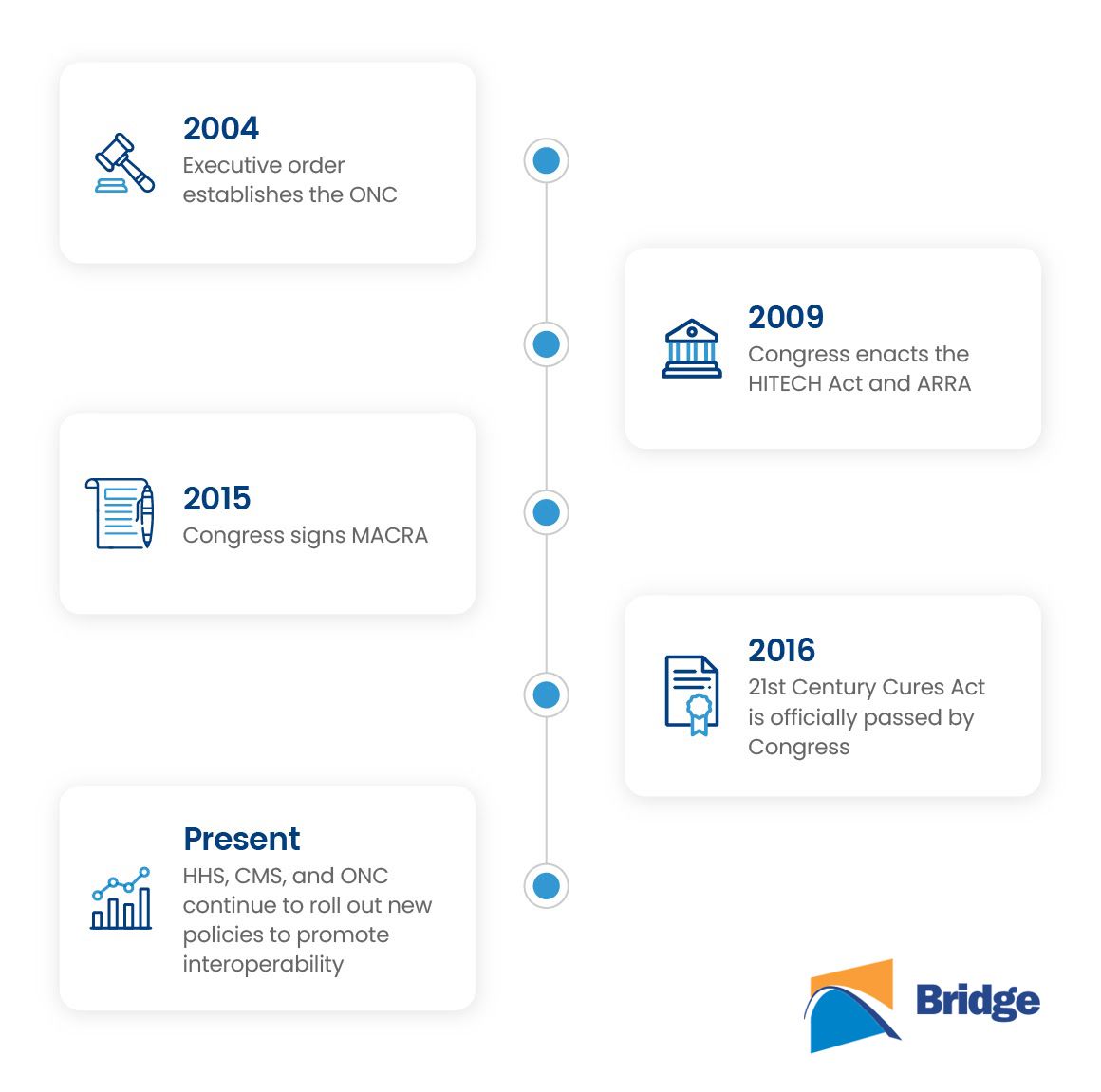
MACRA provides new ways to pay physicians for caring for Medicare beneficiaries. Under MACRA, participating providers will be paid based on the quality and effectiveness of the care they provide. MACRA is one of the four components of MIPS, which combines existing CMS quality programs (including meaningful use)
MIPS is one of the two payment tracks created under MACRA. MIPS adjusts payment based on performance in four performance categories.
Cures Patients should be able to access their electronic medical records at no additional cost. Providers should choose the IT tools to provide the best care for patients without high fees or technical barriers. The CURES act further promotes interoperability. Promoting Interoperability is 25% of the MIPS score. Freeing up and securing clinically relevant data will accelerate the move to a value-based reimbursement model.²⁴ The bipartisan support for both MACRA and the 21st Century Cures Act will force the industry to move from a hospital-based model of care into a patient-centric model and start moving healthcare down the road to personalized precision medicine.
- Wright, J. and Podson, D. (2019). 2019 IPPS Final Rule: Medicare Promoting Interoperability Program Changes. [online] Available at: https://www.cms.gov/Regulations-and-Guidance/Legislation/EHRIncentivePrograms
- Centers for Disease Control and Prevention (2019). Public Health and Promoting Interoperability Programs. [online] CDC. Available at: https://www.cdc.gov/ehrmeaningfuluse/introduction.html
- Federal Register. (2015). Medicare and Medicaid Programs; Electronic Health Record Incentive Program-Stage 3 and Modifications to Meaningful Use in 2015 Through 2017. [online] Available at: https://www.federalregister.gov/documents/2015/10/16/2015-25595/medicare-and-medicaid-programs-electronic-health-record-incentive-program-stage-3-and-modifications.
- www.healthit.gov. (n.d.). How long will the electronic health record incentives opportunity last? | HealthIT.gov. [online] Available at: https://www.healthit.gov/faq/how-long-will-electronic-health-record-incentives-opportunity-last
- qpp.cms.gov. (n.d.). QPP Overview - QPP. [online] Available at:https://qpp.cms.gov/about/qpp-overview
- www.healthit.gov. (n.d.). How long will the electronic health record incentives opportunity last? | HealthIT.gov. [online] Available at: https://www.healthit.gov/faq/how-long-will-electronic-health-record-incentives-opportunity-last
- www.cms.gov. (n.d.). Promoting Interoperability Programs | CMS. [online] Available at: https://www.cms.gov/Regulations-and-Guidance/Legislation/EHRIncentivePrograms/index?redirect=/ehrincentiveprograms/#BOOKMARK2
- Anon, (n.d.). CMS Promoting Interoperability in 2021: All good things must come to an end? – HLN Consulting, LLC. [online] Available at: https://www.hln.com/cms-promoting-interoperability-in-2021-all-good-things-must-come-to-an-end/index.html#:~:text=Promoting%20Interoperability%3A%20Medicaid%20%E2%80%93%20This%20program
- CMS Medicare and Medicaid EHR Incentive Programs Milestone Timeline. (2010). [online] . Available at: https://www.cms.gov/Regulations-and-Guidance/Legislation/EHRIncentivePrograms/Downloads/EHRIncentProgtimeline508V1.pdf
- www.cms.gov. (n.d.). Medicare and Medicaid Promoting Interoperability Program Basics | CMS. [online] Available at: https://www.cms.gov/Regulations-and-Guidance/Legislation/EHRIncentivePrograms/Basics#:~:text=In%202021%20all%20EPs%20will
- Anon, (n.d.). CMS Promoting Interoperability in 2021: All good things must come to an end? – HLN Consulting, LLC. [online] Available at:https://www.hln.com/cms-promoting-interoperability-in-2021-all-good-things-must-come-to-an-end/index.html#:~:text=Promoting%20Interoperability%3A%20Medicaid%20%E2%80%93%20This%20program.
- www.cms.gov. (n.d.). Fiscal Year (FY) 2021 Medicare Hospital Inpatient Prospective Payment System (IPPS) and Long Term Acute Care Hospital (LTCH) Final Rule (CMS-1735-F) | CMS. [online] Available at: https://www.cms.gov/newsroom/fact-sheets/fiscal-year-fy-2021-medicare-hospital-inpatient-prospective-payment-system-ipps-and-long-term-acute-0
- Centers for Medicare and Medicaid Services (CMS) (2013). Medicaid Electronic Health Record Incentive Payments for Eligible Professionals. [online] Available at: https://www.cms.gov/Regulations-and-Guidance/Legislation/EHRIncentivePrograms/Downloads/MLN_MedicaidEHRProgram_TipSheet_EP.pdf
- Centers for Medicare and Medicaid Services (CMS) (2013). Medicaid Electronic Health Record Incentive Payments for Eligible Professionals. [online] Available at: https://www.cms.gov/Regulations-and-Guidance/Legislation/EHRIncentivePrograms/Downloads/MLN_MedicaidEHRProgram_TipSheet_EP.pdf
- Medicare Electronic Health Record Incentive Payments for Eligible Professionals Participation in Other CMS Incentive Programs. (n.d.). [online] . Available at:https://www.cms.gov/Regulations-and-Guidance/Legislation/EHRIncentivePrograms/Downloads/MLN_MedicareEHRProgram_TipSheet_EP.pdf
- www.cms.gov. (n.d.). 2020/2021 Program Requirements Medicaid | CMS. [online] Available at:https://www.cms.gov/regulations-guidance/promoting-interoperability/20202021-program-requirements-medicaid
- www.cms.gov. (n.d.). 2020 Program Requirements Medicare | CMS. [online] Available at:https://www.cms.gov/Regulations-and-Guidance/Legislation/EHRIncentivePrograms/2020ProgramRequirementsMedicare
- ecqi.healthit.gov. (n.d.). Eligible Professional / Eligible Clinician eCQMs | eCQI Resource Center. [online] Available at: https://ecqi.healthit.gov/ep-ec?year=2020
- Anon, (n.d.). CMS Promoting Interoperability in 2021: All good things must come to an end? – HLN Consulting, LLC. [online] Available at:https://www.hln.com/cms-promoting-interoperability-in-2021-all-good-things-must-come-to-an-end/index.html#:~:text=Promoting%20Interoperability%3A%20Medicaid%20%E2%80%93%20This%20program.
- qpp.cms.gov. (n.d.). About Exception Applications - QPP. [online] Available at: https://qpp.cms.gov/mips/exception-applications
- qpp.cms.gov. (n.d.). 2020 Quality Measures. [online] Available at: https://qpp.cms.gov/mips/explore-measures/
- Bonamici, S. (2016). H.R.34 - 114th Congress (2015-2016): 21st Century Cures Act. [online] www.congress.gov. Available at: https://www.congress.gov/bill/114th-congress/house-bill/34
- Federal Register. (2020). 21st Century Cures Act: Interoperability, Information Blocking, and the ONC Health IT Certification Program. [online] Available at: https://www.federalregister.gov/documents/2020/05/01/2020-07419/21st-century-cures-act-interoperability-information-blocking-and-the-onc-health-it-certification.
- Mullin, R. (2017). MACRA, and 21st Century Cures Act Will Drive Interoperability Forward. [online] Health IT Answers. Available at: https://www.healthitanswers.net/macra-21st-century-cures-act-will-drive-interoperability-forward/
- Amazonaws.com. (2017). [online] Available at: https://qpp-cm-prod-content.s3.amazonaws.com/uploads/179/2018%20MIPS%20Scoring%20Guide_Final.pdf
- Amazonaws.com. (2021). [online] Available at: https://qpp-cm-prod-content.s3.amazonaws.com/uploads/0/2019%20MIPS%20Scoring%20Guide.pdf
- Amazonaws.com. (2018). [online] Available at: https://qpp-cm-prod-content.s3.amazonaws.com/uploads/819/2020%20MIPS%20Quick%20Start%20Guide.pdf
- Able Health. (2020). Complete Guide to MIPS 2021: scoring, payment adjustments, measures, and reporting frameworks. [online] Available at: https://ablehealth.com/2020/08/06/complete-guide-to-mips-2021/