ACO Patient Portal and Meaningful Use
- Blake Rodocker
- September 18, 2014
Outdated as of May 2021.
This article is outdated. Please find our updated resource that explains the current MACRA / MIPS / Meaningful Use regulations.
For those not entirely familiar with Accountable Care Organizations, here’s a brief explanation:
Accountable Care Organizations (ACOs) are groups of medical providers who take collective responsibility for the quality, cost and overall care of Medicare patients. The goal of ACOs is for Medicare patients, specifically the chronically ill, to receive high quality care without the duplication of services and medical errors commonly seen in other models. In return for taking this responsibility on, ACO members receive reimbursements when they meet quality metrics and reductions in cost of care. ACOs haven’t completely removed traditional fee-for-service payments, but they offer bonuses when costs are kept down and care quality is high.
ACOs offer a paradigm for a new fee-for-value model – a model that we expect to see most healthcare organizations moving towards in the future.
Trend Towards a Value-Based Model
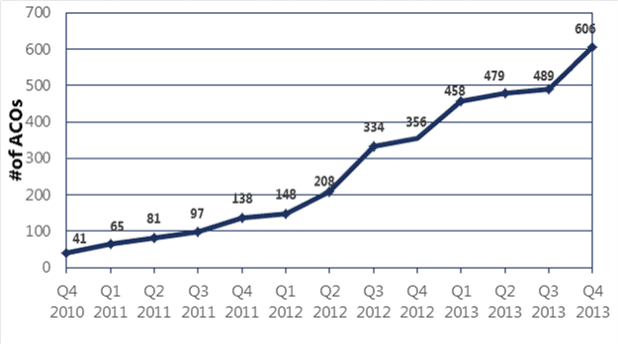
The historical growth of the Accountable Care Organizations market is demonstrated below, with the number of ACOs having increased dramatically between 2010 and 2013. This trend is predicted to continue, with ACOs expected to double by the end of 2014.
Source: Accountable Care Growth in 2014
ACOs and Meaningful Use
There is 58% overlap between the requirements for ACOs and requirements for Meaningful Use – regulations that are affecting all healthcare providers in the U.S. In addition to federal government efforts to shift to a value-based model, shifts have also been happening in the managed care market. There is little doubt that healthcare payment reform is impending. There is general consensus that the U.S. healthcare industry must replace the costly fee-for-service model with something more efficient and high-quality. These major policy trends hint at a larger shift toward a value-based model, and some private sector organizations have even successfully embraced the value-based model. Therefore preparing now to attest for all the Meaningful Use stages will not just allow organizations to receive stimulus dollars, but also prepare them for upcoming changes to reimbursement models.
Patient Portals
Meaningful Use patient portals are an integral tool for ACOs to accomplish their goals. At the most basic level, patient portals enable organizations to qualify for accountable care or wellness incentive payments. In addition, they are becoming a critical tool for providers to keep costs down and quality of care high – the essence of the accountable care model.
A growing body of research studies have proven that participation in an online healthcare portal improves patient engagement.1 Additionally, patients engaged in their own healthcare have proven to have better clinical outcomes.2 The Bipartisan Policy Center reported3 that patient engagement is associated with:
- Reduced diagnostic testing and expenditures
- Fewer referrals
- Fewer elective surgeries
- Increased adherence to prescribed medical treatments
- Increased functional status and faster recovery
- Higher levels of satisfaction
- Higher levels of health literacy
- Higher levels of positive health-related behavior changes
An engaged patient is also critical for an ACO because, unlike traditional Health Maintenance Organizations (HMOs), a patient is not restricted to visiting providers in the ACO network. This means the ACO must do an outstanding job of keeping a patient satisfied and engaged with the providers in the network.
Patient portals help organizations provide care at a lower cost, allowing them to meet the ACO financial requirements. There are basic cost benefits related to efficiency and productivity and more complex benefits as well. Patients can be significantly involved in the delivery of their care and perform tasks without care team assistance. Portals can also allow organizations to contract lower cost staff (i.e. outsourced staff) to assist in the care management remotely. Through more frequent online care, ACOs can avoid readmissions and costly emergency visits.
Sources
1 : https://e-patients.net/archives/2014/08/new-evidence-engaged-activated-patients-do-better-and-cost-less.html
2: The American Journal of Managed Care, March 2012
3: https://bipartisanpolicy.org/sites/default/files/BPC_Engaging_Consumers_Using_Electronic_Tools.pdf